Thrombosis: Permeability
Permeability of Blood Clots:
Plasma hypercoagulability is an established risk factor for thrombosis; however, it is unknown whether abnormal plasma protein levels are a biomarker of pro-inflammatory disease, a causative mechanism in the etiology and therefore a therapeutic target, or both. Using in vitro and in vivo thrombosis models, we have shown that elevated fibrinogen (hyperfibrinogenemia) directly promotes thrombosis by increasing thrombus fibrin content (1). Importantly, we further showed that hyperfibrinogenemia increases thrombus resistance to intravenous thrombolytics (1), demonstrating a novel mechanism to explain the high rate of failure of thrombolytic therapy. These novel findings have important implications for the use of thrombolytic agents in stroke, myocardial infarction, and deep vein thrombosis and the importance of clot permeability relative to these conditions. We hypothesize network structural changes affect clot permeability. Fibrin permeability is used as an explicit measure of fluid transport through the clot and has been correlated with heart disease, stroke, diabetes, and venous thromboembolism.
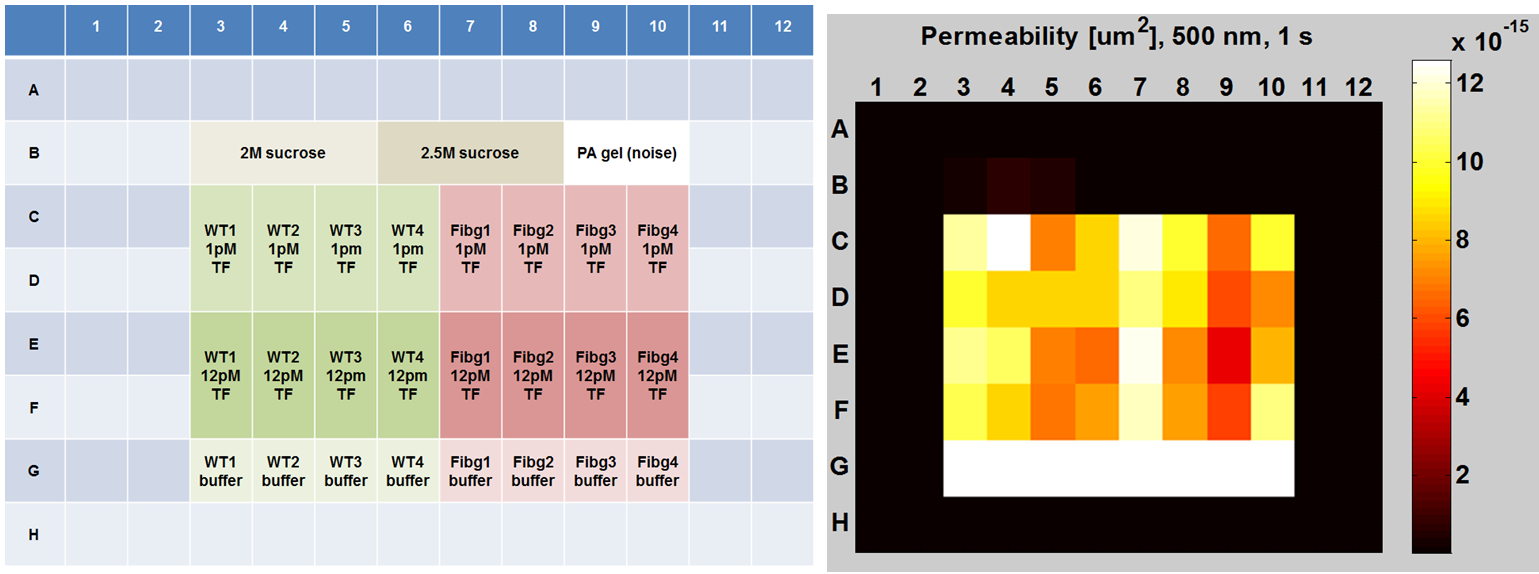
(Left) Experimental plate layout for a murine clotting experiment. (Right) Permeability data for the layout depicted at left. Permeability was determined in each well from bead diffusion data (dozens of beads in multiple locations within each well).
Collaborators:
- Alisa Wolberg, Assistant Professor, Department of Pathology and Lab. Medicine, The University of North Carolina at Chapel Hill. Prof. Wolberg has worked most recently with CISMM in the development of methods assessing structure and permeability of fibrin gels on cell cultures using confocal microscopy and passive microbead diffusion techniques.
- Frank Church, Professor of Pathology and Laboraotory Medicine, UNC-CH.
References:
1. Machlus KR, Cardenas JC, Church FC, Wolberg AS. Causal relationship between hyperfibrinogenemia, thrombosis, and resistance to thrombolysis in mice. Blood. 2011;117(18):4953-63.